 
This program has the lowest income threshold of the four. If you qualify for this program, you automatically qualify for the Extra Help prescription drug program to help you with the out-of-pocket costs of your medicines. The Qualified Medicare Beneficiary (QMB) program helps pay for Part A and Part B premiums as well as deductibles, coinsurance and copays.Each program has specific income and asset limits and eligibility requirements that are adjusted annually. 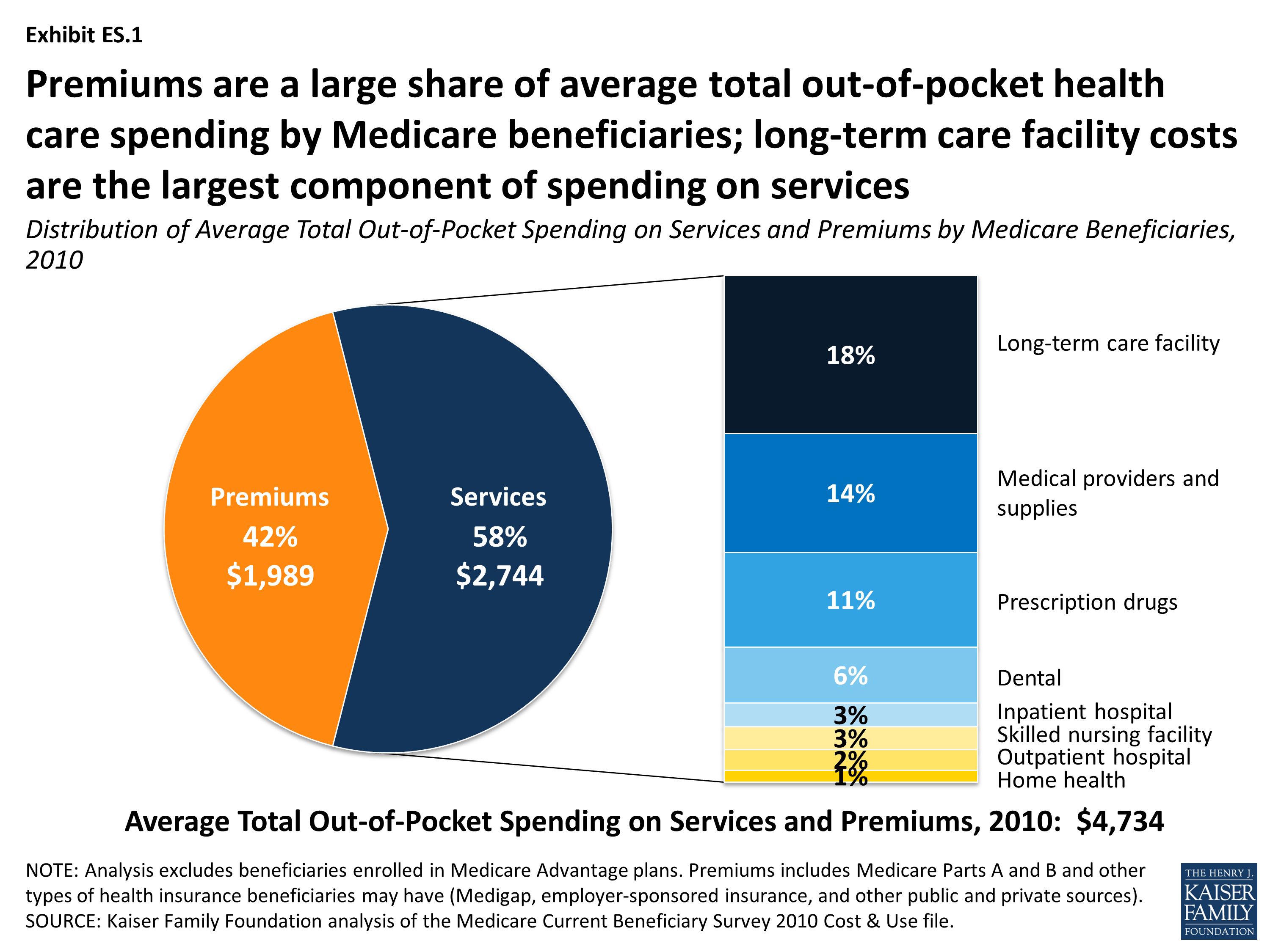
Other programs are designed for beneficiaries with incomes that are too high to qualify for Medicaid but who still have trouble paying their health care bills. Individuals on both Medicare and Medicaid are known as “dual eligibles.” If you qualify for Medicaid, the federal-state health insurance program for people with low incomes and individuals with disabilities, it will pay some or all of your out-of-pocket expenses. If you’re struggling to meet those expenses, you might be eligible for federal and state assistance. We will continue to urge Congress and the Administration to advance such a proposal in their ongoing efforts to better protect the health, financial security, and well-being of everyone who relies on the program.Medicare’s out-of-pocket costs - premiums, deductibles, copays and coinsurance - can easily result in a large tab each year. These updates would greatly improve access and affordability for millions. This cap should also apply to-and be lower than-current MA limits, which are too high. At Medicare Rights, we support limiting beneficiary out-of-pocket costs program wide, including in Part D. This report shows the important benefits and costs of adding a cap to Original Medicare. Using the higher MA cap would cost around $14 billion less but would benefit 2 million fewer beneficiaries than the standalone $5,000 cap. Adding the Part D cap would benefit an additional 200,000 beneficiaries and add $2 billion in Medicare spending. Urban also investigates two other alternatives: adding an out-of-pocket cap of $2,000 to Part D in addition to a general $5,000 limit, and modeling a $7,550 limit, which is the Medicare Advantage (MA) in-network out-of-pocket maximum for 2022. Out-of-pocket spending on Part D would drop by $1 billion (11.4%) while Medicare program spending for OM Part D enrollees would increase by 13.1%. Part D’s portion of this change would be substantial. Across the whole OM population, this cap would decrease their cost sharing by 27.6%, split across out-of-pocket, Medicaid, and Medigap, and increase Medicare program spending by an estimated $1,000 per person (7.8%). This would increase Medicare spending for this population by approximately $8,500 (12.9%) per year. The researchers estimate that a $5,000 cap would cut out-of-pocket, Medicaid, and Medigap spending in half for high-cost beneficiaries. These expenditures are typically covered by out-of-pocket spending or by supplements like Medicaid or Medigap. The report shows that currently, most OM beneficiaries, 32.6 million, face costs below $5,000 per year. Urban investigates what the effect would be of instituting a $5,000 out-of-pocket cap in OM, including Parts A (hospital coverage), B (outpatient coverage), and D (prescription drug coverage). While lower income beneficiaries may be able to enroll in Medicaid or Medicare Savings Programs (MSPs) that reduce their expenses and others might have access to retiree plans or may buy Medigap plans to help cover Medicare costs, many have nowhere to turn for help. The lack of an out-of-pocket limit can leave beneficiaries exposed to unmanageable expenses. It also puts enrollee financial security at risk. This sets this coverage apart from individual Marketplace plans, Medicare Advantage, and most employer-based coverage. The report found that such a change would decrease beneficiary spending, as well as for Medicaid, and supplemental insurance like Medigap, while increasing Medicare program spending.Ĭurrently, people in OM and those with Part D prescription drug coverage do not have any limit to their potential yearly medical costs. Medicare Provider Overpayments Problematic and Point to Larger IssueĮarly this month, the Urban Institute released a report that investigated adding a $5,000 out-of-pocket limit to Original Medicare (OM), and limiting spending by specific payers, including beneficiary out-of-pocket, supplementary coverage plan, and Medicaid.CMS Continues Push for Nursing Home Ownership Transparency.The Inflation Reduction Act’s Part B Insulin Price Takes Effect July 1.HHS Projects Significant Medicare Beneficiary Savings Under the IRA.Administration Looks to Restrict Junk Plans. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
